Treatments for Rosacea
Physical Health
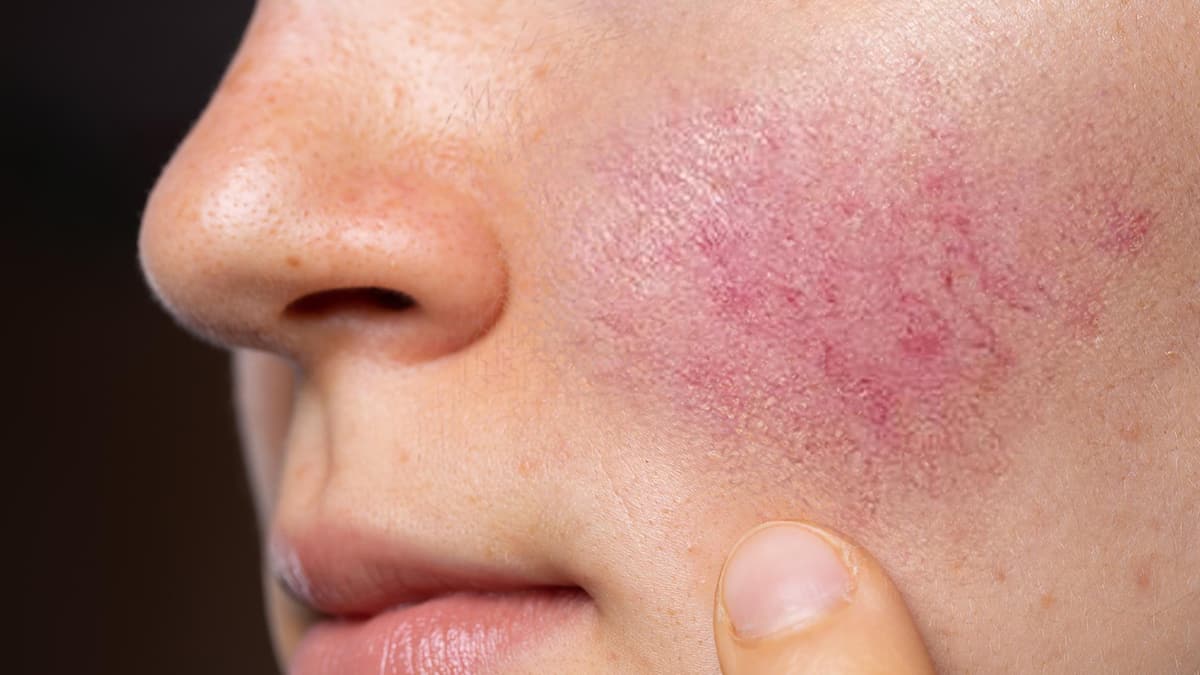
If you’ve recently been diagnosed with the skin condition rosacea, you may be wondering what treatments are available. Rosacea is a common chronic (long-term) skin condition that causes flushing and redness on the face. According to the American Academy of Dermatology (AAD), there are 4 types of rosacea that are defined by the symptoms they cause:
- Erythematototelangiectatic rosacea: Causes flushing, redness, and visible blood vessels
- Phymatous rosacea: Causes skin thickening, giving it a bumpy texture
- Papulopustular rosacea: Causes breakouts similar to acne, leading to redness and swelling
- Ocular rosacea: Causes irritation and redness in the eyes, along with eyelid swelling
Living with a visible skin condition like rosacea can be difficult for some. A survey by the National Rosacea Society (NRS) found that 9 out of 10 people with rosacea say their condition affects their personal appearance and lowers their self-confidence and self-esteem.
It’s important to work closely with your healthcare provider or dermatologist (skin specialist) to find the best treatment plan for your rosacea symptoms. The types of treatment you’ll use depend on your symptoms and what areas of your skin they affect.
This article will cover the most common rosacea treatments, when they’re used, and any side effects you should know about. For more information about your treatment plan, talk to your dermatologist.
Treatments for Skin Redness and Flushing
Skin redness and flushing are often the most obvious signs of rosacea. These symptoms usually start on the nose and spread out toward the cheeks. You may also have visible spider veins or tiny, broken blood vessels that sit just below your skin. People with rosacea tend to blush or flush more easily compared to those without the condition. These symptoms can be embarrassing for some — fortunately, there are several treatment options available to help.
Topical Medications
If you have mild or moderate rosacea with redness and flushing, your dermatologist may prescribe a topical treatment. Brimonidine (Mirvaso®) and oxymetazoline (Rhofade®) are prescription medications approved by the United States Food & Drug Administration (FDA) for treating rosacea. Both medications work by targeting blood vessels, causing them to narrow or constrict. By limiting blood flow through the blood vessels in the face, brimonidine and oxymetazoline help limit skin redness and flushing.
Mirvaso is available as a topical gel that’s applied to the affected skin once daily or as needed. Its effects usually last 3-6 hours. Rhofade is available as a topical cream applied to the affected skin once daily or as needed. It lasts much longer than brimonidine, usually up to 12 hours.
The most common side effects of Mirvaso and Rhofade are temporary and include:
- Skin redness and flushing
- Allergic reactions (contact dermatitis), which can cause skin itching and pain
- Worsening of rosacea pimples
Ask your dermatologist or pharmacist about your insurance coverage for Mirvaso and Rhofade since many insurance plans don’t cover the costs of these medications.
Light Therapy
Light therapy may be used alongside topical or oral medications for treating visible spider veins and thickened skin from rosacea. Lasers are intense, focused beams of light used to target leaky blood vessels or to resurface layers of thickened skin. Common types of laser treatment for rosacea include pulsed dye laser therapy and neodymium:yttrium-aluminum-garnet (Nd:YAG) laser therapy.
Intense pulsed light (IPL) therapy is a non-laser treatment that uses lamps to create high-intensity light pulses. IPL therapy is used to treat rosacea, spider veins, and wrinkles.
The AAD notes that most people see a 50-75% improvement in their spider veins within the first 3 light therapy treatments. You can expect the results to last between 3-5 years. On the other hand, thickened skin tends to return over time, even after multiple rounds of light therapy. It’s best to seek treatment sooner rather than later for the best results.
Common side effects of laser therapy typically clear within 1-2 weeks of treatment and include:
- Red or irritated skin
- Red or purple spots or rashes
- Itchy, tight, or painful skin
It’s important to protect your skin from the sun following light therapy treatment. It’ll be particularly sensitive to burns and scarring while it heals. Be sure to follow some tips below about proper sunscreen application while living with rosacea.
Lifestyle Modifications
When living with rosacea, it’s important to take extra steps to protect your skin. Exposure to sunlight is the leading cause of rosacea flare-ups that lead to red, flushed skin. Be sure to apply broad-spectrum sunscreen regularly when you’re out in the sun with a sun protection factor (SPF) of at least 30. Some sunscreens may irritate your sensitive skin, so try looking for ones that contain zinc oxide and/or titanium dioxide. Try to avoid going out in direct sunlight during the middle of the day when the sun is strongest. If you do have to be outside, cover your face with a sunhat or use an umbrella.
Your dermatologist may also recommend using gentle skincare products to avoid irritating your skin and triggering redness. Look for a mild, non-soap cleanser that has a neutral pH. Use only your fingertips to apply cleanser and wash your skin. Rinse with lukewarm water and gently pat your face with a clean towel to dry. The NRS recommends waiting 30 minutes before applying any topical medications after washing your face to avoid stinging and irritation. After applying medications, wait an additional 5-10 minutes to apply sunscreen, gentle moisturizer, or makeup.
Treatments for Rosacea Skin Bumps

Many people with rosacea also develop raised red skin bumps (papules) that may be filled with pus (pimples or pustules). These bumps usually form on the central area of the face, affecting the nose, cheeks, forehead, and chin. Your dermatologist may prescribe a topical or oral medication for your symptoms, depending on how severe they are and what areas of your skin are affected.
Topical Medications
There are several topicals for treating papules and pustules with rosacea.
Azelaic acid is an anti-inflammatory molecule with antioxidant properties for treating mild-to-moderate rosacea, acne, and other skin conditions. Your dermatologist may prescribe azelaic acid as a foam (Finacea® Foam) or gel applied twice daily to the skin. Most people apply it once in the morning and again in the evening. Common side effects include skin burning and tingling, which typically go away over time. You may also notice that areas of your skin become lighter than others. If you notice this side effect, talk to your dermatologist right away.
Another topical used for mild-to-moderate rosacea is encapsulated benzoyl peroxide cream (Epsolay®). This cream is specially formulated to treat sensitive skin without drying it out. Benzoyl peroxide targets acne-causing bacteria responsible for pustules in rosacea. Your dermatologist will have you apply Epsolay once daily. Common side effects include skin pain, redness, swelling, and itching. Since the benzoyl peroxide is encapsulated, you likely won’t experience any stinging, burning, dryness, scaling, or itching.
For moderate-to-severe rosacea, dermatologists may prescribe topical ivermectin (Soolantra). This medication helps reduce skin inflammation in rosacea. Doctors also believe Soolantra acts as an anti-parasitic by targeting the Demodex mite. These mites live on the skin and may make rosacea symptoms worse. Soolantra comes as a cream that’s applied in a thin layer on the skin once daily. Common side effects include dry or irritated skin, burning sensations, and itchiness.
In 2020, the FDA approved minocycline topical foam (Zilxi®) for reducing papules and pustules with rosacea. Minocycline is a topical antibiotic with anti-inflammatory properties. Your dermatologist will have you apply Zilxi once daily. When taken by mouth, minocycline can have several unwanted side effects. However, clinical studies with the topical form in Zilxi show that it’s safe and effective. Diarrhea was the most commonly reported side effect.
Topical metronidazole has been used for over 60 years to treat papules and pustules with rosacea. It’s commonly prescribed as a cream or gel that’s applied once or twice daily. Metronidazole is an antibiotic, but researchers think it works by reducing inflammation in the skin. Dermatologists prescribe metronidazole as a lotion, gel, or cream that’s applied once or twice daily. Common side effects include skin burning, dryness, itching, and stinging.
The combination of sulfacetamide sodium and sulfur has long been used to treat a variety of skin conditions, including rosacea, seborrheic dermatitis, and acne. Your dermatologist may prescribe a specific strength of sulfacetamide sodium and sulfur as a gel or cream. You can find these ingredients in over-the-counter cleansers. Before trying sulfacetamide sodium and sulfur, be sure to let your dermatologist know if:
- You’re sensitive to sulfur
- You have kidney disease
- You’re pregnant or planning on becoming pregnant in the near future
Side effects to be aware of include temporary redness, dryness, irritation, and itching.
Oral Medications
When topical treatments for rosacea aren’t effective, dermatologists prescribe oral medications instead. The FDA has approved low-dose oral doxycycline (Oracea®) for treating papules and pustules with rosacea. While doxycycline is an antibiotic, it doesn’t work by killing bacteria. Instead, it helps reduce inflammation contributing to skin bumps. Oracea is a 40-milligram (mg) capsule taken once daily in the morning. Your dermatologist will have you take it 1 hour before or 2 hours after eating breakfast. Please note that this medication can make your skin more sensitive to the sun.
Treatments for Thickened Skin With Rosacea
Phymatous rosacea causes skin thickening and rough, bumpy skin. These skin changes are known as phyma, and they’re caused by enlarged sebaceous glands. The sebaceous glands release sebum, an oily substance that lubricates the skin’s surface. Phymatous rosacea is common in men and typically affects the nose — known as rhinophyma. However, phyma can also affect the chin and cheeks.
The best way to prevent phyma is to start treatment as soon as possible. Your dermatologist may have a harder time treating thickened skin, as it continues to worsen over time. If you have rhinophyma, you’ll likely be prescribed oral isotretinoin. This medication is approved for treating severe acne and works by reducing the size of sebaceous glands. Studies show early treatment with isotretinoin can help reduce skin thickening on the nose.
Some people with phymatous rosacea may not respond to isotretinoin treatment. Your dermatologist may recommend surgery to remove thickened areas of skin. They’ll use a scalpel to carefully remove the extra skin. After the surgery, they’ll use other techniques to help smooth and shape the skin. Your dermatologist will choose a method they’re familiar with to give you the best results.
If surgery isn’t the best option for you, your dermatologist may recommend laser therapy. Treatment with an Nd:YAG laser vaporizes the skin to destroy sebaceous glands. Laser therapy is also used to target spider veins and reduce redness in phymatous rosacea.
After your surgery, you may need to take isotretinoin for an extended period of time to prevent your skin from thickening again. It’s also important to work with your dermatologist to find your rosacea triggers and avoid them.
Treatments for Ocular Rosacea
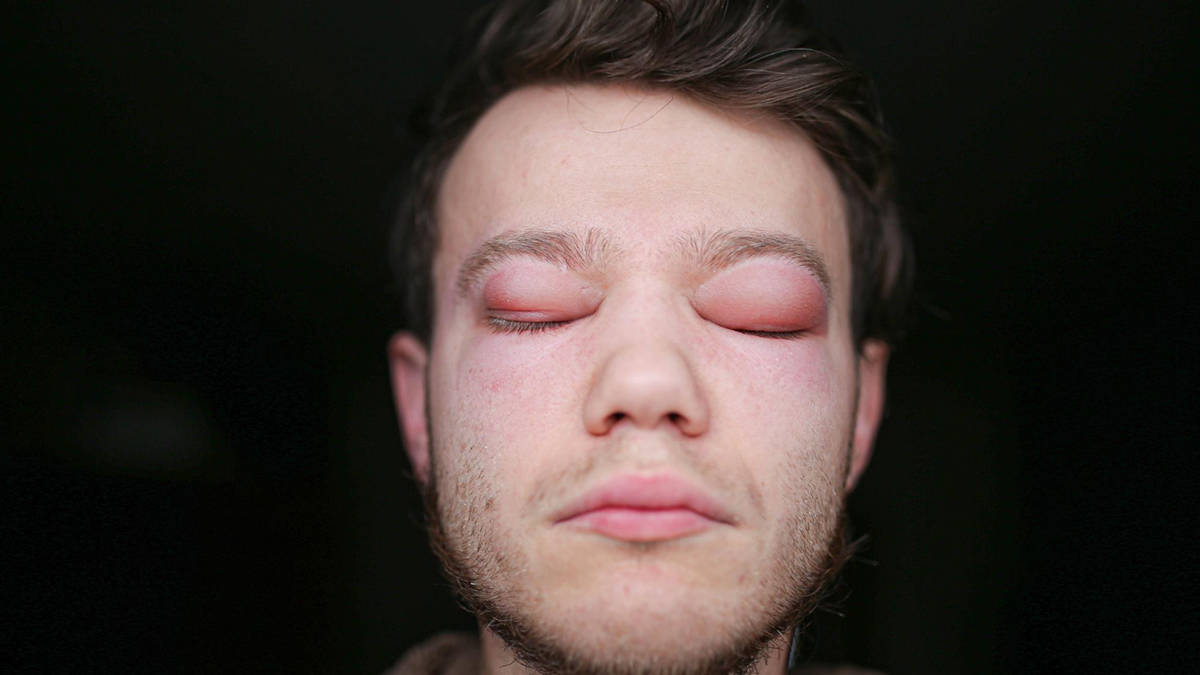
Over half of people with cutaneous rosacea (skin symptoms) also have ocular rosacea affecting their eyes. At first, you may think your symptoms are caused by old contact lenses, allergies, or changing seasons. Common symptoms include:
- Swollen, red eyelids
- Inflammation in the outer layer of your eye (conjunctivitis)
- Crusts on your eyelashes or eyelids
- Red or bloodshot eyes
- Itching or burning sensations in your eyes
- Sensitivity to light
- Feeling like something is in your eye
- Dry eyes or excessive tearing
If you’re experiencing long-term eye symptoms living with rosacea, it’s time to make an appointment with your eye doctor (ophthalmologist). They can prescribe treatments based on how severe your symptoms are. It’s important to stick to your treatment plan as closely as possible to avoid developing problems with your eyesight.
Medicated eye drops with steroids help treat inflammation, redness, and swelling. Gentle eyelid scrubs are formulated to keep your eyes clean and prevent infections. Your ophthalmologist may also recommend artificial tears, which can be found over the counter at your local pharmacy or drug store. You can also apply a warm compress using a clean washcloth dipped in warm water and placed over your eyes.
Your dermatologist and ophthalmologist may work together to ensure your rosacea treatment plan is working. Some rosacea treatments — like antibiotics — can treat both skin and eye problems.